Ultimate Guide to Ventilation for Airborne Pathogen Control

Ventilation is one of the most effective tools for reducing airborne pathogens in healthcare and caregiving environments. It helps dilute contaminated air, directs airflow to contain pathogens, and filters harmful particles. Key strategies include ensuring proper air changes per hour (ACH), maintaining directional airflow, and using high-efficiency filtration systems like HEPA filters.
Here’s what you need to know:
- Air Changes per Hour (ACH): Isolation rooms require 12 ACH, while general patient rooms need at least 6 ACH.
- Directional Airflow: Negative pressure in isolation rooms prevents pathogens from escaping, while positive pressure protects sterile spaces.
- Filtration: HEPA filters capture 99.97% of particles as small as 0.3 microns, while MERV 13–16 filters work for broader HVAC systems.
- Supplementary Measures: Portable HEPA units, upper-room UVGI systems, and proper exhaust systems improve air quality, especially during outbreaks.
Ventilation works best when paired with careful room layouts, reduced fabric disturbance during care tasks, and regular system maintenance. These measures create safer spaces for patients and caregivers alike.
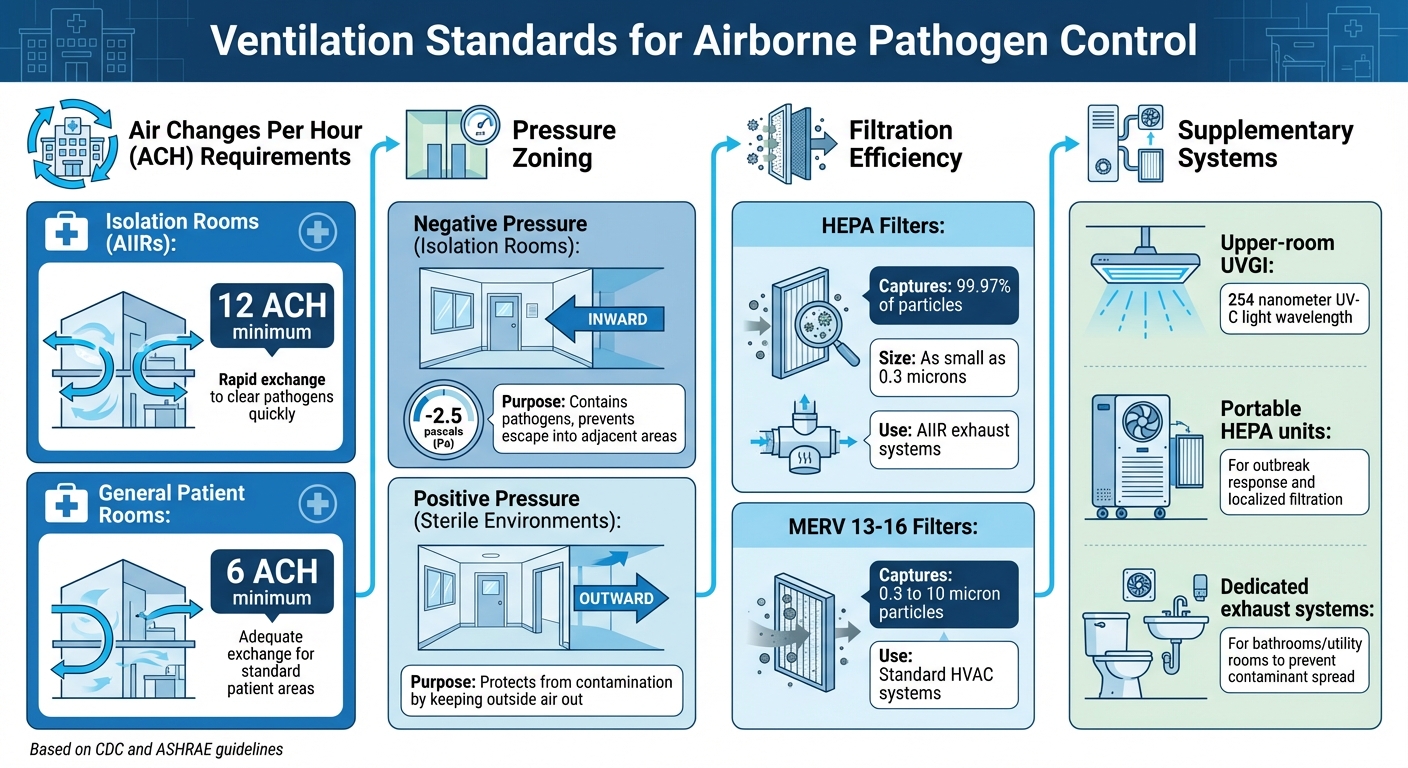
Ventilation Requirements and Filtration Standards for Healthcare Pathogen Control
Ventilation and Infection Control in Healthcare
Core Principles of Ventilation for Pathogen Control
Ventilation plays a key role in controlling the spread of airborne pathogens. To create a safer environment, three main strategies work hand-in-hand: diluting contaminated air, directing airflow from clean to dirty areas, and filtering out pathogens before they can spread further. Together, these methods build multiple layers of defense against airborne transmission, especially in healthcare settings. Let’s start with a foundational concept: air changes.
Air Changes per Hour (ACH) Explained
Air Changes per Hour (ACH) measures how many times the total air volume in a room is replaced with fresh air within an hour. For example, the CDC recommends 12 ACH for airborne infection isolation rooms (AIIRs) in acute-care facilities, ensuring efficient dilution of airborne pathogens. In comparison, general patient rooms require at least 6 ACH [1]. Studies, like those by Menzies and colleagues, show that lower ACH rates correlate with higher rates of tuberculin conversion among healthcare workers, highlighting the direct link between inadequate ventilation and increased infection risk [2]. Increasing ventilation rates beyond ASHRAE 62.1 standards can further reduce the spread of airborne pathogens by expelling contaminants more quickly, especially in shared spaces [2][4].
Directional Airflow and Pressure Zoning
Directional airflow ensures air moves strategically through a facility, always flowing from clean zones to areas with greater contamination risk. In isolation rooms, negative pressure creates an inward pull, containing pathogens and preventing them from escaping into hallways or nearby spaces. AIIRs maintain a pressure difference of approximately -2.5 pascals (Pa) compared to surrounding areas, and exhaust air is filtered through HEPA systems before being released [1][2]. On the other hand, positive pressure protects sterile environments by pushing air outward, keeping contaminants from entering. However, poor construction or maintenance can disrupt these airflow patterns, increasing the risk of transmission [2][6]. In general wards, exhaust vents in bathrooms are often used to maintain a clean-to-dirty airflow pattern throughout the space. While managing airflow is crucial, capturing any remaining pathogens is equally important.
Filtration and Air Cleaning Systems
HEPA filters are highly effective, capturing 99.97% of particles as small as 0.3 microns. They are essential in AIIR exhaust systems, trapping droplet nuclei before air exits the room [1][3]. In standard HVAC systems, MERV-rated filters (MERV 13–16) are used to capture particles ranging from 0.3 to 10 microns, preventing pathogens from recirculating in broader areas [1][4]. Routine inspections of filters are critical. According to ASHRAE and NADCA guidelines, HEPA filters should be replaced when the pressure drop exceeds 2–3 inches of water gauge, and coils and ducts should be regularly cleaned to avoid pathogen buildup [1][4].
Upper-room UVGI systems use UV-C light at a wavelength of 254 nanometers to inactivate airborne microbes. As HVAC fans circulate air through the treated zone, UVGI provides an additional layer of protection. The CDC notes that UVGI is particularly effective in high-risk areas, as it extends exposure time to the light, reducing viable pathogens without relying solely on high ACH [3][7][8]. Many healthcare facilities have taken steps to improve their HVAC systems by incorporating UV disinfection and upgrading to higher-rated filtration during renovations or new construction projects [3].
Ventilation Strategies for Caregiving and Healthcare Environments
Effective ventilation in healthcare settings isn’t a one-size-fits-all approach. Different areas - shared care spaces, high-risk zones, and utility rooms - require specific strategies to manage airborne pathogens and maintain a safe environment.
Ventilation in Shared Care Areas
Shared spaces, like waiting rooms and general care areas, present a higher risk of pathogen transmission before patients are isolated. The primary goal here is to dilute contaminated air quickly while preventing airflow from spreading pathogens between individuals. To achieve this, supply diffusers should be positioned above or behind workstations, directing clean air across the room toward exhaust grilles located either overhead or near the floor. Beds should always be placed away from supply vents to avoid exhaled air being blown across occupants [2].
In waiting areas and day rooms, ventilation rates higher than the minimum code requirements are especially helpful during respiratory illness seasons [5]. Pairing increased outdoor air intake with MERV 13 or higher filters in central HVAC systems can trap fine aerosols effectively. While privacy curtains offer visual separation, they can disrupt air patterns and should not replace proper airflow design. Physical separation between beds remains a more reliable infection control measure [2]. When structural changes aren't feasible, portable HEPA units can supplement central ventilation, especially during outbreaks in crowded spaces [3][8].
Isolation Rooms and High-Risk Zones
Airborne infection isolation rooms (AIIRs) are designed to contain pathogens using negative pressure, at least 12 air changes per hour (ACH), and HEPA filtration [1][5]. These rooms require precise calculations to maintain 12 ACH, with exhaust air ideally vented directly outdoors. If recirculation is unavoidable, HEPA filters must treat the air before it re-enters the building [1][5]. Sealed doors and tight penetrations are critical to maintaining airflow and pressure balance [1].
During patient surges, single-patient rooms equipped with exhaust fans vented outdoors or portable HEPA units can be converted into temporary isolation spaces. However, these setups demand continuous pressure monitoring and strict door-closing policies to ensure effectiveness. Unlike engineered AIIRs, these improvised spaces are more vulnerable to human error and maintenance lapses [1][5][8].
Ventilation for Bathrooms and Laundry Areas
Bathrooms and soiled utility rooms can release aerosols during toilet flushing or while handling contaminated linens. Dedicated exhaust systems ensure negative pressure relative to adjacent hallways, preventing odors, moisture, and bioaerosols from spreading into patient care areas [5][7]. Exhaust fans should vent directly outdoors - not into interior spaces or plenums - and provide adequate air changes to remove contaminants quickly [5][7]. Keeping doors closed is essential to maintaining this negative pressure.
In laundry areas, it’s important to separate airflow between dirty receiving areas and clean folding zones to prevent cross-contamination. Staff should handle soiled linens in ventilated, negatively pressured utility rooms rather than in hallways or shared spaces. To minimize aerosolization, soiled items should be handled gently and placed in covered bins near local exhausts [2][5]. Disposable multi-layer bedding systems, such as PeelAways, can also help limit handling. These systems allow caregivers to peel away a soiled layer instead of performing full linen changes, reducing the risk of aerosol generation during incontinence care.
Combining Ventilation with Bedding and Incontinence Care
Bringing together effective ventilation systems with smart bedding practices significantly reduces the risk of infection. Even the most advanced ventilation can’t eliminate pathogens that never become airborne. That’s where thoughtful bedding choices and well-organized workflows come into play. By limiting the disturbance of contaminated fabrics during routine care, caregivers help ventilation systems maintain low levels of airborne pathogens.
Reducing Exposure During Bed Changes
Minimizing the agitation of contaminated linens is a key part of infection control and ties directly into ventilation strategies. Traditional bed-changing methods - like pulling, snapping, or folding linens - can release particles into the air. On top of that, moving soiled linens through hallways can spread contaminants before ventilation systems have a chance to clear the particles. Products like PeelAways multi-layer disposable sheets tackle this issue by allowing caregivers to remove soiled layers right at the bedside. This peel-away method reduces handling and eliminates the need to transport contaminated linens, minimizing the risk of particles becoming airborne again. This combination of ventilation and reduced fabric disruption creates a safer environment during bed changes.
Workflow Strategies for Shared Rooms
In shared or semi-private rooms, timing and task sequencing are critical to managing infection risks. Before starting a bed change, caregivers should ensure that air supply vents and exhaust grilles are clear and that bathroom exhaust fans are running. Closing corridor doors and positioning privacy curtains to avoid blocking airflow can further enhance the control of airborne particles. Care routines should prioritize noninfected individuals first, with strict adherence to hygiene and PPE protocols to prevent cross-contamination. The streamlined process of using PeelAways not only reduces bedside activity time but also gives ventilation systems more time to clear any particles stirred up during care.
Benefits of Disposable Multi-Layer Bedding
The design of PeelAways simplifies bed changes with a single peel-away motion, often completing the task in under a minute. This eliminates the need for mattress lifting or linen folding, both of which can disturb contaminants. Each layer - typically 5 to 7 waterproof sheets - blocks liquids while still allowing airflow, helping to contain accidents and keep the mattress cleaner. This low-disruption process aligns perfectly with ventilation protocols, reducing exposure time and improving infection control efforts.
sbb-itb-45288fe
Monitoring and Maintaining Ventilation Systems
Even the best ventilation systems can falter without consistent oversight. Keeping an eye on critical metrics is essential to prevent potential issues. Regular maintenance not only ensures smooth airflow but also plays a key role in safeguarding residents and staff from airborne pathogens. Let’s dive into the routine checks and practices needed to keep these systems running at their best.
Key Ventilation Metrics to Track
One of the most important metrics to monitor is air changes per hour (ACH). For airborne infection isolation rooms (AIIRs), the CDC recommends a minimum of 12 ACH [1]. Another crucial factor is maintaining proper differential pressure, which prevents contaminated air from leaking into adjacent areas. Filter performance is equally important - especially in high-risk zones. HEPA filters, for instance, are designed to capture 99.97% of particles as small as 0.3 microns. Monitoring the pressure drop across these filters can signal when it’s time for a replacement [1].
Routine Testing and Maintenance Practices
Daily checks should verify that pressure monitors are functioning correctly and that air grilles remain clear of obstructions. In high-risk areas, methods like smoke tests can confirm proper airflow direction. Additionally, ensure exhaust fans in spaces like bathrooms and utility rooms are working as intended.
On a quarterly or semiannual schedule, professional testing and balancing are essential. This process involves recalculating airflow rates, confirming ACH, and adjusting dampers to ensure the system meets infection-control standards. Regular cleaning of components like coils, drain pans, and humidifiers helps prevent microbial growth. Lastly, annual calibration of sensors and monitoring devices is necessary to ensure reliable readings for infection-control measures.
Adjusting Ventilation During Outbreaks
During outbreaks, ventilation systems may need temporary adjustments to meet heightened demands. For respiratory illnesses like COVID-19 or influenza, increasing outdoor air ventilation above the usual minimum can dilute pathogen concentrations indoors. Isolation rooms should be closely monitored to ensure they maintain their target ACH and negative pressure levels. Portable HEPA units can be deployed in shared spaces, such as break rooms, for added air cleaning.
To further reduce risks, ventilation systems can be run for extended periods before and after occupancy, effectively flushing indoor air. Disabling demand-control strategies that lower ventilation based on occupancy can also help maintain higher airflow during outbreaks. Rapid checks of pressure relationships, exhaust system performance in critical areas like bathrooms, and timely filter replacements should all be prioritized when pathogen loads increase. These steps ensure the system is prepared to handle the added strain during such events.
Conclusion
Ventilation plays a critical role in reducing airborne pathogens within caregiving and healthcare environments. Systems designed to provide at least 12 air changes per hour, maintain proper airflow direction from clean to dirty zones, and incorporate HEPA filtration can significantly reduce pathogen levels in the air. However, ventilation alone isn't a complete solution.
To enhance these efforts, improving bedding workflows is another key step in minimizing contamination risks. As mentioned earlier, caregivers are often exposed to airborne and surface contaminants during high-contact tasks. This is where disposable multi-layer bedding, such as PeelAways, offers a practical advantage. These innovative sheets reduce fabric disturbance during bed changes, preventing contaminated linens from resuspending dried particles into the air. With over 12,000 satisfied customers and a 4.8-star average rating, caregivers frequently highlight the convenience of PeelAways. Jalene Stanger noted that they eliminate the need for "15 loads of laundry and wet mattresses" while maintaining a cleaner, less strenuous caregiving environment.
Comprehensive infection control requires integrating ventilation, filtration, and pressure management strategies. Simple actions like running exhaust fans during care tasks, using smoke tests to confirm airflow direction, and staying on top of filter changes are essential. During outbreaks, increasing outdoor air circulation, ensuring isolation rooms maintain negative pressure, and spacing high-risk activities to allow ventilation systems time to clear the air are crucial steps. Together, these tactics form a well-rounded defense.
For caregivers and facility managers in the U.S., effective infection control comes from pairing robust ventilation with streamlined caregiving practices. Ventilation systems dilute and remove airborne pathogens, but their success depends on proper maintenance and support from aligned workflows. By combining strong airflow, efficient bedding solutions, regular system checks, and consistent staff training, you can create a safer environment for both residents and caregivers.
Related Articles
Pairing effective ventilation with smart bedding protocols and hygiene practices can significantly cut down on contamination risks. Proper ventilation supports care routines by reducing airborne particles during tasks like bed changes and incontinence care. To build on these strategies, check out these articles for more infection-control methods.
These resources dive deeper into bedding solutions and workflow adjustments that work hand-in-hand with ventilation systems.
Top Bedding Solutions for Infection Control
This article highlights bedding options like disposable multi-layer systems, waterproof covers, and fluid-resistant protectors designed to reduce aerosol release during linen changes. It explains how these choices can limit fabric disturbance, helping to keep particles out of the air. The article also includes examples tailored for U.S. nursing homes, assisted living facilities, and home-care environments, accounting for varying HVAC capabilities and budgets.
How to Reduce Cross-Contamination in Caregiving Settings
This article focuses on applying ventilation strategies to daily caregiving tasks, offering workflows that lower the risk of cross-contamination. Topics include scheduling care tasks to align with ventilation cycles, creating movement patterns that follow clean-to-dirty principles, and handling soiled bedding to minimize particle resuspension. It also provides practical checklists for U.S. long-term care facilities, hospitals, and home-care environments, making it easier to integrate these methods into staff routines.
The Role of Disposable Bedding in Elder Care
This article discusses how disposable bedding systems play a vital role in infection control, especially in elder care settings where residents are more vulnerable and HVAC systems may be outdated. It outlines how products like PeelAways reduce the handling of soiled linens, cutting down on airborne and contact contamination risks. Caregiver and facility examples demonstrate how disposable bedding fits seamlessly into infection-control plans alongside ventilation and filtration efforts.
FAQs
What is Air Changes per Hour (ACH), and how does it help control infections in healthcare facilities?
Air Changes per Hour (ACH) refers to the number of times the air within a room is completely replaced with fresh air over the course of an hour. A higher ACH is especially important in healthcare environments, as it helps reduce the presence of airborne pathogens, improves overall ventilation, and decreases the likelihood of airborne illnesses spreading.
Boosting ACH levels allows healthcare facilities to maintain safer spaces for patients, staff, and caregivers, particularly in high-risk areas such as hospitals and clinics where infection control is a top priority.
How does directional airflow help reduce the spread of airborne pathogens?
Controlling how air flows within a space is a key strategy in reducing the spread of airborne pathogens. Directional airflow helps by guiding contaminated air away from clean areas and ensuring it exits the building, rather than lingering indoors.
With tools like exhaust systems and proper ventilation in place, effective airflow patterns can greatly lower the chances of cross-contamination, making indoor spaces safer for everyone.
How do portable HEPA filters and UVGI systems improve indoor air quality during outbreaks?
Portable HEPA filters and UVGI (Ultraviolet Germicidal Irradiation) systems play a crucial role in improving indoor air quality by tackling harmful particles and pathogens in the air. HEPA filters are designed to trap microscopic contaminants, while UVGI systems take it a step further by neutralizing bacteria, viruses, and other microorganisms through ultraviolet light.
These technologies are particularly useful during outbreaks, as they help lower the risk of airborne transmission, making indoor spaces safer. By complementing existing ventilation systems, they work together to deliver cleaner and healthier air.
Related Blog Posts
Comments
0

SAVE MONEY & WATER
Professionals & Institutions save a fortune on labor/laundry.

SUPERIOR COMFORT
The first thing our customers notice is how soft our sheets are.

100% WATERPROOF
Each layer is 100% Waterproof, perfect for spills and accidents

SAVE TIME
Change the sheet in under 1 minute without stripping the bed.




Leave a comment