How to Reduce Laundry Costs in Your Care Facility: 10 Proven Strategies

Laundry is one of the biggest expenses in care facilities, with labor making up 40–50% of costs and linen replacement adding another 15–25%. But detergent, often blamed, accounts for just 3–7%. To cut costs effectively, focus on labor, energy, and textile management. Here are 10 actionable strategies:
- Conduct linen audits to track the true cost per wash.
- Set clear linen policies to minimize waste and misuse.
- Monitor usage by department for better accountability.
- Upgrade to energy-efficient equipment to save on utilities.
- Optimize water and energy use with simple adjustments.
- Compare reusable vs. disposable bedding and use PeelAways to reduce laundry loads.
- Buy in bulk and manage inventory smartly to lower supply costs.
- Train staff on efficient laundry practices to reduce rewashes.
- Subscribe to PeelAways for consistent savings.
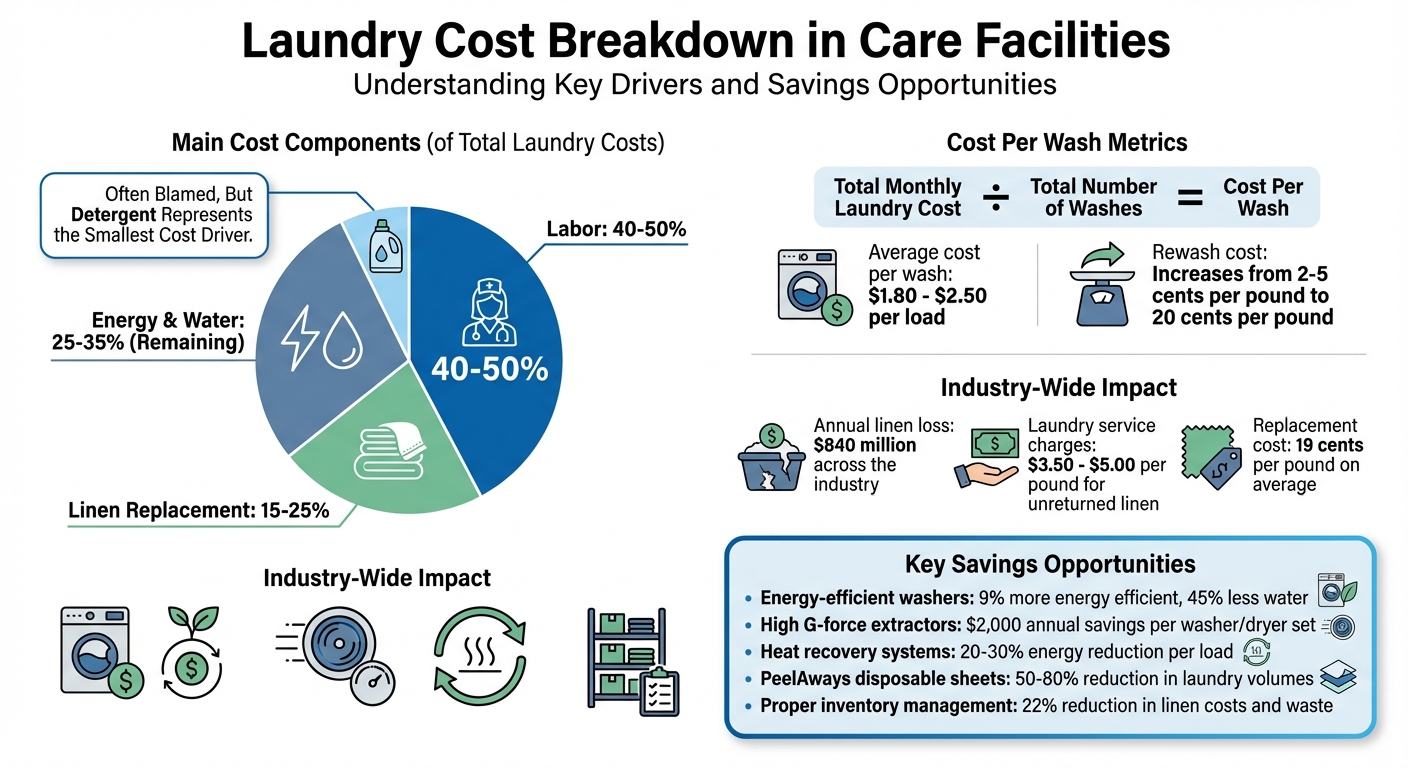
Laundry Cost Breakdown in Care Facilities: Where Your Budget Goes
Strategy 1: Conduct Regular Linen Audits
Regular linen audits are key to uncovering waste, overstocking, and unnecessary expenses in laundry operations. These audits help you assess the true cost per wash, factoring in labor, energy, water, chemicals, and textile replacement. Myles Cook, Sales Director at Able, highlights the importance of this metric:
"Understanding your cost per wash is one of the most accurate ways to measure laundry efficiency in a care home".
To calculate your baseline cost, use this straightforward formula:
Total monthly laundry cost ÷ Total number of washes = Cost per wash.
In U.S. care facilities, the cost per wash typically falls between $1.80 and $2.50 per load. Breaking down these costs reveals that labor often makes up 40%–50% of the total, textile replacement accounts for 15%–25%, and detergent represents only 3%–7%. This granular understanding of expenses lays the groundwork for additional cost-saving measures for laundry.
Uncovering Hidden Losses
Physical audits are essential for identifying inventory loss. For example, staff may stash linens in unauthorized locations to avoid shortages, leading to hidden losses. Regular checks can help recover these misplaced items. Eric Frederick, a healthcare laundry expert, emphasizes another effective approach:
"Billing the end-user for linen usage has proven effective in reducing the amount of linen used, as well as the associated replacement costs due to theft or abuse".
Billing end-users directly encourages mindful usage, reducing waste and replacement expenses.
Monitor Key Metrics
Tracking the soil-to-clean ratio is another valuable practice. This involves comparing the weight of clean linen delivered to the weight of soiled linen returned. Any significant discrepancies could indicate loss or improper disposal. Additionally, keep an eye on your rewash rates - high rates often point to inefficient equipment or poor wash chemistry, wasting both labor and energy.
To maintain accountability, conduct monthly internal audits and quarterly supplier reviews. These consistent evaluations ensure that inefficiencies and hidden losses are addressed promptly, forming a strong foundation for broader cost-saving strategies.
sbb-itb-45288fe
Strategy 2: Establish Clear Linen Usage Policies
Clear linen usage policies help staff manage linen more efficiently, reducing unnecessary laundering and waste. These guidelines should address handling procedures, bed change frequency, containment protocols, and storage standards. When staff recognize that linen is a hospital resource with a specific cost, they naturally adopt more mindful practices.
Accurate cost assessments lay the groundwork for these policies, which streamline operations further. Start by implementing standardized handling procedures. For example, staff should always roll soiled linen carefully to avoid spreading contaminants - shaking linen is a strict no-go. The CDC advises:
"Carefully roll up soiled linen to prevent contamination of the air, surfaces, and cleaning staff. Do not shake linen".
Additionally, solid waste must be scraped into a commode using a firm instrument before the linen is bagged. Soiled linens should always be placed in clearly labeled, leak-proof containers at the point of use and never carried against the body.
Bed change frequency is another key factor. Establish clear guidelines to avoid both under-laundering and waste. For occupied beds, change linens at least once daily, and for new patient admissions, ensure fresh linens are provided. For patients who are bedridden or unable to maintain personal hygiene, increase the frequency beyond the daily standard. This approach strikes a balance between infection control and cost management.
Set proper laundering standards as well: wash linens at 158–176°F (70–80°C) for 10 minutes, ensuring optimal load volumes. Store clean linens in designated areas and transport them in carts cleaned daily to avoid contamination from dust or debris, which could lead to unnecessary re-laundering. Healthcare laundry experts Mark Whitten and Phil Charlton emphasize:
"Linens that are cleaned thoroughly and handled correctly can help prevent these costs [HAIs], while also preventing the development and spread of superbugs".
Staff training is essential to reinforce these policies. Form a linen committee with representatives from various units, environmental services, and infection control to identify and address weak points. Post visual Standard Operating Procedures (SOPs) in laundry areas and patient care rooms to serve as reminders. Some facilities have successfully implemented "Linen Awareness Day" programs to educate staff on proper linen usage. These initiatives address an industry-wide issue that results in $840 million annually in linen loss. By adopting these measures, facilities can improve accountability and reduce waste effectively.
Strategy 3: Track Linen Usage by Department
After implementing regular audits and clear usage policies, tracking linen usage by department is the next step to tighten cost control. By monitoring how each department uses linen, you can reduce waste and promote accountability. When staff understands that linen is a budgeted hospital supply - with a defined cost - rather than a free resource, overuse and waste naturally decrease. Plus, this tracking makes it easier to identify where losses are happening.
Linen loss is a persistent issue in the U.S. healthcare system, with laundry services charging $3.50–$5.00 per pound for unreturned linen. Eric Frederick, a healthcare laundry consultant, emphasizes the importance of shifting perceptions:
"The key to these reductions is the ability to get the end-users to see linen as a hospital supply with a defined cost, instead of a free item".
One effective tool is soil-to-clean ratio tracking, which compares the weight of clean linen delivered to the weight of soiled linen returned. This method reveals items that aren’t cycling back into the laundry system, often due to being stored in departments instead of being returned. Dan Sanchez, President of Sanchez Advisory Group, puts it bluntly:
"Linen loss is 'money being thrown into the fire'".
Unaccounted-for linen adds up quickly, with replacement costs averaging around 19 cents per pound.
Another way to reduce waste is by assigning linen costs to specific departments. When areas like nursing, the ER, or the OR are responsible for budgeting their linen usage - just as they do with other medical supplies - department heads become more conscious of consumption. Tracking also helps identify misuse, such as staff using bath blankets for fluid absorption. Some facilities have curbed overuse by changing delivery methods, like bagging washcloths by weight instead of stacking them, which discourages staff from taking more than necessary.
To further enhance accountability, establish a linen committee with representatives from key areas like medical units, environmental services, infection control, and security. This group also ensures that cost-saving measures align with laundry hygiene standards to maintain resident safety. This committee reviews usage data, identifies department-specific waste, and promotes shared responsibility for linen management. By turning linen usage into a collaborative effort, hospitals can significantly improve their operations and reduce unnecessary expenses.
Strategy 4: Upgrade to Energy-Efficient Laundry Equipment
Switching to energy-efficient laundry equipment can cut down on water, energy, and detergent costs while also helping linens last longer. For example, Energy Star-certified commercial washers are about 9% more energy-efficient and use roughly 45% less water than standard models. Features like moisture sensors, high-capacity front-loaders, and smart technology can further drive down expenses.
These upgrades not only improve efficiency but also deliver noticeable savings. High G-force extractors are a great example - they remove more water during the spin cycle, which shortens drying times. And since drying is the most expensive part of laundry operations, this can make a big difference. Bill Brooks, National Sales Manager at UniMac, highlights this point:
"Tumble dryers account for 70% of a laundry operation's utility expenses, so anywhere drying times can be reduced will alleviate costs".
By reducing drying time by an average of 10 minutes per load, a single washer/dryer set could save about $2,000 annually in natural gas costs.
Advanced washers also come equipped with conductivity sensors, which check for detergent residue and cut down on unnecessary rinse cycles. This feature alone can lower water use by 15–30%. Similarly, moisture sensors in dryers help prevent over-drying, saving energy and protecting linens. Bill Smith, Director of Operations for Aramark’s South Central Region, explains:
"Moisture sensors in dryers are great. There is the energy component, of course, but also, there is less damage to garments and linens if over-drying is eliminated".
Eliminating just eight minutes of over-drying in a 75-pound dryer can save nearly $900 in utility costs and $5,000 in labor annually.
When choosing equipment, consider front-loading washers without agitators - they handle larger loads more gently. Look for spray rinse technology, which can reduce water use by 11%–39%. Ozone laundry systems are another option, as they sanitize linens in cold water and can cut hot water usage by as much as 75%.
Before making a purchase, check with local utility companies for rebates or incentives. Many utilities offer financial assistance for facilities upgrading to Energy Star-rated equipment. You can search for programs by ZIP code using the Database of State Incentives for Renewables & Efficiency (DSIRE) or the Energy Star Rebate Finder tool. While energy-efficient machines may cost about $2,000 more upfront, they typically pay for themselves through long-term savings on utilities and labor. These upgrades are an effective way to reduce costs in care facilities.
Strategy 5: Reduce Water and Energy Consumption
Fine-tuning operational settings can significantly boost savings beyond just upgrading equipment. By adjusting wash cycles, temperature settings, and maintenance schedules, facilities can lower water and energy costs by as much as 30–50%, all while maintaining hygiene standards. These changes are low-cost to implement but deliver ongoing savings that quickly add up.
Start by optimizing wash temperatures. Lowering default settings from 194°F to 104–140°F can slash water heating expenses by 30–50%. Modern detergents remain effective at these lower temperatures, ensuring infection control is not compromised. For heavily soiled or contaminated linens, thermal disinfection at 160–180°F should only be used when necessary, rather than as the default for every load. These adjustments, combined with equipment upgrades, create a well-rounded approach to cutting energy and water costs.
Load sizing plays a key role in efficiency. Filling washers to 80–90% capacity prevents underloading, which wastes resources, and overloading, which leads to longer cycles due to inefficient rinsing. Auto-dosing systems can further improve efficiency by dispensing the right amount of detergent based on load size and soil level. This reduces rewashes and prevents detergent residue. Pairing optimized cycle loads with scheduling cycles during off-peak hours adds another layer of energy savings.
Speaking of scheduling, running high-energy cycles during off-peak hours can take advantage of reduced utility rates. Additionally, installing pressure-reducing valves to maintain water pressure at 30–50 PSI can cut water waste by 5–10%. For dryers, daily cleaning of lint traps and monthly professional duct cleaning can prevent energy-draining buildup, ensuring machines run efficiently.
Another impactful upgrade is heat recovery systems, which capture hot air expelled by dryers. This can lower energy consumption by 20–30% per load. As ACE Laundry explains:
"Efficiency ratings only tell part of the story. The real savings come from how those machines are used, how water and energy flow through your facility, and how well your staff is trained".
Strategy 6: Use PeelAways Multi-Layer Disposable Bed Sheets

Disposable bedding options like PeelAways can significantly cut down laundry needs while slashing labor costs, making them a practical addition to earlier energy-saving measures.
PeelAways multi-layer disposable bed sheets reduce laundry volumes by 50–80% and cut bed-changing time from 15 minutes to under 60 seconds. Each sheet features 5–7 waterproof layers that peel away individually when soiled, revealing a fresh layer underneath - all without needing to move the patient.
This system eliminates the need for traditional laundering. Since every layer is completely waterproof, it protects mattresses from fluids, stains, and odors, which helps extend their lifespan and reduces the need for replacements. For facilities dealing with frequent bed changes or streamlining incontinence care tasks, this solution also lowers utility bills and labor demands. It’s a simple way to ease the workload while improving care efficiency.
How PeelAways Simplifies Bed Changes
Changing traditional bed sheets involves lifting patients, stripping linens, and remaking the bed - a process that takes about 15 minutes and often strains caregivers. PeelAways simplify this by allowing staff to peel off the soiled top layer in under a minute, all while the patient stays comfortably in bed. This eliminates heavy lifting and reduces the physical strain on caregivers, lowering the risk of workplace injuries.
The sheets are tailored for standard hospital beds in Twin XL size, a common choice for care facilities. Each layer can last 7 to 10 days if it remains clean, and the bamboo/rayon blend delivers a soft, breathable feel - far from the stiff, crinkly texture of some disposable options. As Sarah, a caregiver, shared:
"PeelAways have been a game-changer for me and my mother. The ease of changing the sheets has saved me so much time and energy, and my mother feels more comfortable and dignified."
This streamlined process not only reduces physical effort but also drives significant cost efficiencies.
Cost Savings with PeelAways
PeelAways can cut labor costs by approximately 66%, reducing the cost per bed change from $6.25 to $2.08 (based on a $25/hour wage). And unlike traditional linens, which cost about $0.60 per pound to launder, PeelAways eliminate laundry expenses altogether. For a 100-bed facility, the annual savings can range from $200,000 to $500,000, with a return on investment achieved in 3–12 months.
Additionally, the waterproof layers protect mattresses from fluid damage, eliminating the need for separate mattress protectors and avoiding premature replacements that can cost anywhere from $500 to $3,000 per unit. John, a home health aide, emphasized:
"As a professional caregiver, PeelAways are indispensable. They make my job easier and my clients happier. The ability to quickly change sheets without disturbing my clients is invaluable."
Strategy 7: Buy in Bulk and Manage Inventory Effectively
Buying linens and detergents in bulk can help cut down per-unit costs while also reducing the time spent on procurement and keeping costs stable. The trick is to pair these volume discounts with solid inventory management to avoid overstocking or running out of essential supplies. This approach supports earlier cost-saving measures by extending savings from operations to supply procurement.
Bulk purchases allow you to lock in prices for six to 12 months, shield against inflation or supply chain disruptions, and consolidate shipments to save on delivery fees. Instead of paying multiple delivery charges for smaller, frequent orders, you pay just one. Plus, investing in durable linens that can withstand industrial laundering reduces waste and lowers replacement expenses over time.
Start by conducting a one-month usage audit to gauge how much your facility truly needs. This prevents overstocking items that could sit unused or expire - like disinfectants and sanitizers, which often have a shelf life of only 1–2 years. Once you know your usage rates, set up automated deliveries to save time and labor. For instance, if an employee spends two hours weekly managing supply runs, that adds up to over $2,000 annually in labor costs at $20 per hour.
To maximize the benefits of bulk buying, combine it with precise inventory tracking. Monthly tracking of cases or pallets can help minimize errors and keep operations smooth. A dedicated inventory system can reduce linen costs and waste by as much as 22%, ensuring your bulk purchases bring value without overloading your storage or tying up funds unnecessarily.
Make sure your storage is climate-controlled and choose linens that can handle frequent, high-temperature washing. This minimizes wear and tear, lowering the total cost of ownership. By combining bulk purchasing with effective inventory management, you not only save money but also enhance the overall efficiency of your operations.
Strategy 8: Train Staff on Efficient Laundry Practices
Teaching your staff effective laundry techniques can significantly lower rewash rates and labor costs, which together make up 40–50% of your total laundry expenses. This is a key step in reducing operating costs while improving care for residents. Focus on training your team to sort laundry correctly, load machines to 90% capacity, and handle stains immediately. These steps help avoid costly rewashes, which can increase processing costs from just 2–5 cents per pound to a steep 20 cents per pound. As American Laundry News aptly notes:
"Nothing kills the efficiency of an operation faster than doing a load of laundry … and then doing it again".
Start with pre-sorting. Experts agree that sorting linens properly before washing is 75% of the solution to reducing rewashes. Train housekeeping staff to separate heavily soiled items into specific bags before they reach the laundry room. This prevents stains from becoming permanent during the drying process, which often requires harsh chemicals to remove - damaging fabrics and shortening the lifespan of your linens. In long-term care facilities, a rewash rate above 2–3% typically signals a need for better training.
Visual aids can make a big difference. Place posters or loading charts near machines to remind staff of best practices during every shift. For example, use a chart that translates bag counts into weights - like "three blue bags = 50 lbs" - so employees can load washers to the recommended 90% capacity without guesswork. Underloading wastes water and energy, while overloading can trap dirt in folds, leading to rewashes. A small floor scale in the laundry room can also help staff ensure proper machine loading.
Building new habits takes time. Studies show it takes about 66 days of consistent practice to form lasting habits in linen management. To support this, hold short "QuickCare" training sessions and back them up with newsletters, online modules, or even screensavers featuring key reminders.
Cross-training staff on multiple tasks, like sorting and loading, can also improve efficiency. This flexibility ensures smooth operations during staff shortages or busy periods without relying on overtime. It also gives employees a better understanding of how their role impacts the entire laundry cycle. Facilities that implement a clear, one-way laundry flow - keeping dirty and clean linens separate - have reported a 10% drop in infection rates. This shows that solid training not only protects your budget but also safeguards residents' health. A well-trained team ensures consistent, efficient laundry practices across your facility.
Strategy 9: Subscribe to PeelAways for Ongoing Savings
PeelAways offers a subscription service that helps you save 15% on every order, provides free shipping on purchases over $100, and includes a 30-day money-back guarantee. This setup not only reduces your bedding costs but also simplifies budgeting and ensures a steady supply.
You can choose from several delivery intervals - 7, 14, 30, 45, or 60 days - making it easy to align shipments with your facility’s needs. Subscribing automatically applies the discount to every order. For instance, a 50-bed facility ordering Twin XL sheets (regularly priced at $41.99 each) twice a month would pay just $35.69 per sheet with the subscription discount. That’s a savings of about $6.30 per sheet, adding up to over $3,000 annually if 500 sheets are replaced each year. This subscription model transforms fluctuating bedding expenses into predictable costs, complementing other strategies to lower labor and laundry expenses. Plus, free shipping on orders over $100 eliminates freight charges, which could otherwise range from $20 to $50 per shipment.
The 30-day money-back guarantee ensures a risk-free trial. If the sheets don’t meet your facility’s hygiene or workflow standards, aligning with your infection control protocols, you can return any unused items for a full refund. You’ll also receive an email reminder three days before each shipment, allowing you to pause, adjust, or cancel orders through the subscription dashboard if occupancy rates change or inventory builds up.
Many facilities report saving between $5,000 and $10,000 annually by combining the subscription discount with reduced laundry and labor costs. Best of all, there’s no long-term commitment - you can adjust or cancel your subscription anytime to fit your facility’s changing needs.
Conclusion
Cutting laundry costs in your care facility doesn’t have to mean sacrificing hygiene or patient comfort. The 10 strategies outlined here tackle the main cost drivers - labor, textile replacement, and energy use. By conducting regular linen audits, setting clear usage guidelines, investing in energy-efficient equipment, training staff, and monitoring departmental usage, you can lay the groundwork for long-term savings. As Myles Cook, Sales Director at Able, points out:
"Labour and textile replacement usually represent the largest cost components".
Targeting these areas can lead to the greatest financial impact. One standout solution among these strategies is PeelAways, which offers a quick and effective way to save.
PeelAways multi-layer disposable bed sheets reduce bed-change times from 15–20 minutes to just 60 seconds. This not only saves time but also sidesteps the disposable vs. washable bed sheets "cost per wash" cycle, which includes energy, water, chemicals, and fabric wear. Facilities adopting PeelAways can see immediate savings that pair well with other efficiency measures, like energy-efficient upgrades and optimized laundry workflows.
To uncover hidden inefficiencies, calculate your real cost per wash by dividing your total monthly laundry expenses by the number of washes. Then, focus on strategies that minimize the number of times staff handle linens, as labor is the largest expense. Healthcare laundry expert Eric Frederick underscores this point:
"The most efficient way to produce linen is to do it right the first time".
FAQs
What’s the fastest way to calculate our real cost per wash?
To figure out your real cost per wash, start by calculating your cost per wash cycle. Add together all your expenses, including direct costs like labor, chemicals, and utilities, as well as indirect costs such as linen replacement. Then, divide the total by the number of wash cycles completed or the total pounds of laundry processed. This straightforward approach gives you a clear picture of your laundry costs and can highlight areas where you might save money - no complicated math required.
How can we cut laundry labor without lowering hygiene standards?
To make laundry tasks less time-consuming while ensuring hygiene, focus on simplifying processes and using effective tools like disposable sheets. These sheets cut down on handling time and help reduce the risk of cross-contamination. Another smart approach is setting up clear, one-way routes for handling dirty and clean linens. This eliminates unnecessary movement and delays. Together, these methods can save time, lighten the workload, and maintain high hygiene standards in care facilities.
When does switching to PeelAways make the most financial sense?
Switching to PeelAways makes the most financial sense in high-turnover care settings where linens need frequent changing. In these environments, the costs of laundry, labor, and linen replacements can add up quickly. By cutting down on washing and handling expenses, PeelAways can offset their upfront cost in no time, particularly in places where traditional linens are swapped out daily.
Related Blog Posts
Comments
0

SAVE MONEY & WATER
Professionals & Institutions save a fortune on labor/laundry.

SUPERIOR COMFORT
The first thing our customers notice is how soft our sheets are.

100% WATERPROOF
Each layer is 100% Waterproof, perfect for spills and accidents

SAVE TIME
Change the sheet in under 1 minute without stripping the bed.




Leave a comment